Adding Depression to the List of Serious Health Conditions Caused by Chronic Inflammation
The Role of Matrix Metalloproteinases (MMPs)
In the last Briefing, I tied osteoarthritis and diabetes together by advancing an evidence-based hypothesis that chronic low-grade generalized inflammation caused by obesity, defined as exceeding one’s personal fat threshold, is the driver of both conditions (as well as a host of other common chronic non-infectious diseases that affect the heart, liver, and kidneys). This Health and Science Briefing adds new information to that discussion and extends the theoretical argument centering inflammation as the driver of yet another common chronic non-infectious disease, major depression, while identifying a second common source of chronic low-grade inflammation, psychological/emotional stress.
Recap of the Last Briefing
In the last Health and Science Briefing, I included a hyperlink to this study which lays out in detail how the pathological changes seen in the joints of patients with osteoarthritis (OA), including cartilage erosion, disc destruction, and synovial tissue thickening, are mediated by a complex network of biochemical processes coordinated by the so-called 'hormones of the immune system' – small proteins known as cytokines that control local tissue inflammatory responses. These inflammatory cytokines up-regulate the gene expression of a class of proteolytic enzymes (enzymes that degrade protein) called matrix metalloproteinases (MMPs). MMPs act to break down the protein-rix extracellular matrix that gives structural and functional support to our internal organs, and one such MMP, called MMP-13, degrades the protein-rich cartilage and disc structures in joints while simultaneously blunting the biochemical pathways that lead to healing and restoration of those tissues.
In short, obesity causes the chronic production of inflammatory cytokines, inflammatory cytokines stimulate the production of MMP-13, and chronic up-regulation of MMP-13 degrades joint structures and prevents them from healing, leading over time to OA.
I also discussed how obesity is not well defined by BMI but is better understood as a more nuanced and individualized concept of fat accumulation that exceeds a person’s capacity for safe energy storage in subcutaneous adipose tissue (the fat beneath our skin). Each person has a different capacity for how much fat they can safely store subcutaneously and this is known as their personal fat threshold (PFT). Crossing one’s PFT puts stress on and ultimately causes injury to fat cells (adipocytes), stimulating the release of inflammatory immune cytokines such as interleukins and TNF-alpha which attract specialized white blood cells called monocytes to the area of injury to help clean up and render the local adipose tissues temporarily resistant to insulin as a mechanism for self-protection.
Finally, I described a causal link between chronic low-grade generalized inflammation (CLGI) caused by exceeding the personal fat threshold (hereafter: obesity-induced CLGI) and type-II diabetes, OA, and a host of other common chronic illnesses, noting that the same inflammatory cytokines that attract monocytes and induce insulin resistance in adipose tissues also up-regulate the expression of MMP-13 in joints.
In short, chronic obesity that exceeds the personal fat threshold drives CLGI, and CLGI results in chronic insulin resistance, eventually leading to type-II diabetes (T2D) as well as the up-regulation of MMP-13 in joints, leading to OA.
CLGI and Depression
This Briefing expands our understanding of the source of CLGI beyond obesity to include psycho-emotional stress, and our understanding of the wide-ranging health consequences of CLGI beyond OA, T2D, and chronic heart, liver, and kidney disease, to include major depressive disorder.
It has been established that many stress-related psychiatric illnesses such as schizophrenia, bipolar disorder, anxiety disorder, and depression are associated with CLGI as evidenced by elevated circulating levels of inflammatory cytokines, MMP, and monocytes in the blood of patients with these mental health conditions. There is even a growing consensus around the hypothesis that stress-induced CLGI may be a driver of depression. But so far, most of the evidence for this hypothesis has come from studies showing an association between CLGI and depression, and not from randomized controlled studies that are best designed to evaluate causation. Let’s take a moment to unpack this important distinction:
Association and Correlation vs. Cause and Effect
There are several different kinds of scientific studies. In the world of medical research, causality is best established by randomized controlled trials (RCTs) in which participants are randomly assigned to either a treatment or control group. The treatment group receives an intervention while the control group does not. The impact of the intervention is then measured by differences in outcomes between the two groups.
Another way to investigate causality is by conducting what is called an interventional study or clinical trial. Clinical trials are studies in which participants are prospectively (not randomly) assigned to either receive an intervention (the treatment arm) or not (the placebo arm) so that researchers can evaluate the effects of the intervention on biomedical or health-related outcomes. Clinical trials suffer from lack of randomization which can lead to biased outcomes but this problem can sometimes be overcome, at least to some degree, if the study is large enough.
While RCTs and interventional studies are the best ways to establish causality, they can be difficult to perform and often cannot be undertaken for logistical, financial, ethical, or other reasons, leading researchers to instead perform what are called observational studies. Observational studies do not include a control group or the randomization of subjects into treatment and non-treatment arms, and fail to account for hazards like confounding variables and selection bias. In some cases, observation studies rely on data that have not been validated (such as in studies that use self-reported diet information). Most of what health professionals ‘know’ about the effects of diet and nutritional supplementation, for example, comes from studies using this kind of unreliable data.
In short, observational studies are non-experimental, typically uncontrolled studies that are susceptible to external factors that can influence the relationship between exposure and outcome. These limitations significantly reduce the reliability and therefore the scientific value of the findings of observational studies but sometimes they are all we have to go on…
Observational studies look for associations and correlations between independent variables. In research, an association is a general relationship between two variables (for example, when we see X, we also see Y), while a correlation describes a more linear relationship between the variables (for example, when X goes up, Y goes up commensurately, and when X goes down, Y goes down commensurately).
We know that elevated levels of inflammatory cytokines and symptoms of depression are associated with one another because they are reliably observed together. But just because two things are associated (or even correlated) with one another, that doesn’t mean that one causes the other. Elevated levels of inflammatory cytokines might cause symptoms of depression but, with only observational data to go on, it could work the other way around – that depression causes inflammation. It could also be true that both things are caused by a third independent variable (obesity or some other factor might drive both inflammation and depression). And it could also be quite possible that the association between inflammation and depression is simply a matter of coincidence. This is true of all associations and correlations which are the endpoints of observational studies.
To illustrate the point, we see an almost perfect correlation over time between the consumption of margarine and the rate of divorce in the State of Maine:
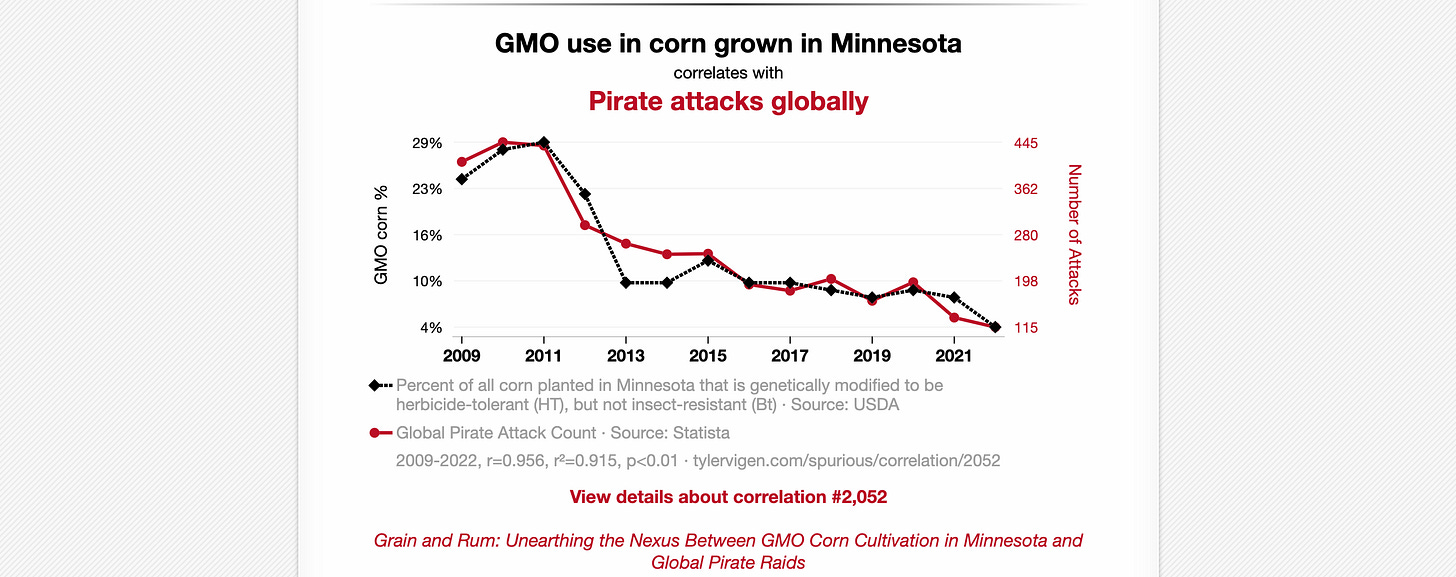
…and the amount of genetically modified corn grown in Minnesota correlates almost perfectly with the rate of worldwide pirate attacks:
Associations and correlations established by observational studies can sometimes be misleading. Disinformation peddlers routinely use the findings of observational studies to bolster false narratives on social media platforms, and news journalists lacking sufficient scientific training (or seeking attention-grabbing headlines) routinely report the findings of observational studies as though they were indicative of causation.
Now, no one really thinks that consuming too much margarine causes divorce or that growing more GMO corn in Minnesota causes increased rates of piracy on the high seas – no matter how striking those correlations may be – and we are unlikely to read about such things in the media or the scientific literature. However, it has been widely reported, based almost exclusively on observational studies, that eating a lot of red meat causes heart disease and colon cancer. Such and understanding has, in fact, become a mainstream belief among experts in the medical and scientific communities, informs the understanding of most physicians (including most cardiologists) today.
And yet, while they are often (but not always) associated with one another in large cohort studies (cohort studies are a kind of observational study), there is almost no evidence that consuming red meat causes either heart disease or cancer. In a major review published in the journal Annals of Internal Medicine, multiple systematic reviews looking at the effects of red (and also processed) meat on common chronic health conditions including heart disease, cancer, and diabetes, found low to very low evidence that either red meat or processed meat is harmful, and concluded that there is no health-related reason to reduce red meat or processed meat consumption. That’s a problem. We rely on medical and scientific experts to be using science properly and that means avoiding the temptation to leap from association to causation.
A recent review of this problem led experts to conclude that unconscious biases rooted in preconceived beliefs about the harmful effects of meat consumption, and not rational data analysis and interpretation, best explains why so many researchers continue to conclude from observational studies that red meat is unhealthy, and why, therefore, cutting down on beef consumption continues to be one of the most common lifestyle recommendations promoted by health professionals across disciplines. In short, as I have been saying for some time, there are good reasons to cut down on or stop eating meat. Animal cruelty is embedded in commercial farming and the raising of animals for slaughter has profound impacts on the environment. But it is not rational or evidence-based to tell patients that eating less meat will improve their health.
Stress, CLGI, and Depression
Returning to depression, last week, a new study published in Nature showed that up-regulating the gene expression of a particular MMP called MMP-8 induces depression-associated behaviors in an animal model. Elevated levels of MMP-8 have already been strongly associated with depression in humans but, as we know, an association does not establish cause-and-effect. In this animal study, chronic stress-induced systemic immune system activation (elevated levels of inflammatory cytokines in the blood), up-regulated MMP-8 expression, affected brain structure and function, and induced metabolic syndrome, gastrointestinal disturbances, and social avoidance and isolation behaviors consistent with depression.
Mirroring the effects on adipose and joint tissues caused by obesity-induced CLGI, stress-induced CLGI caused the migration of monocytes into the vascular system of the brain, particularly in reward centers such as the nucleus accumbens which plays an integral role in addiction and depression. Once in the brain, these monocytes up-regulated their genetic expression of MMP-8 which induced the degradation and abnormal restructuring of the net-like, protein-rich matrix that protects and provides structural and functional support for nerve cells in the brain.
To prove that up-regulating MMP-8 and the resulting erosion of the extracellular matrix in reward centers of the brain was the cause of the observed depression-associated behaviors and not just an associated phenomenon, the ability to express MMP-8 was removed from some of the mice. The mouse portion of the study included two arms: normal mice (the controls) and knockdown mice (with the gene for MMP expression blocked). Compared to the control mice, the knockdown animals did not undergo degradation of their brains’ extracellular matrix, nor did they exhibit self-isolation or social avoidance behaviors associated with major depression when placed under identical conditions of chronic stress. This study offers the first compelling evidence for the theory that stress-induced CLGI, through its upregulation of MMP-8, may be a cause of depression.
A Unifying Theory of Chronic Non-Infectious Disease: CLGI Drives MMP and MMP Drives Many Chronic Diseases by Degrading the Protein-Rich Extracellular Matrix of Organs
The extracellular matrix (ECM) is the proteinaceous material (rich in collagen and elastin) that holds organs together and supports their proper functioning. In addition to providing the essential physical scaffolding for the cellular constituents of an organ, making a kidney look like a kidney, a brain look like a brain, etc., the ECM is a reservoir of growth factors and bioactive molecules that and initiate crucial biochemical and biomechanical activities required for tissue growth, cellular differentiation and maturation, and organ homeostasis (the body's ability to maintain a stable internal environment despite changes in external conditions through dynamic equilibrium). Abnormal ECM dynamics lead to deregulated cell proliferation, failure of cell death, and loss of cell differentiation, resulting in functional defects and pathological processes including tissue fibrosis and cancer.
MMPs degrade ECM which is important for repair and remodeling when cells grow too old (senescence) or are injured (for example after an infection). Such up-regulation of MMP however is meant to be short-lived. Chronic over-expression of MMP driven by CLGI leads over time to the progressive degradation of ECM, the dysregulation of organ tissue function, and the establishment of disease – something that has been well-documented in a wide array of chronic health conditions.
The risks for arterial plaque formation, clotting, and heart attacks are dramatically increased when MMP-9 is chronically elevated in response to obesity-induced CLGI. Statins, used routinely in patients with high cholesterol to lower their risk of heart disease, are, in fact, believed to work in part by down-regulating the expression of MMP-9. Therapies that act to suppress MMP are a major line of research in cancer treatment. As reported in the last Briefing, the chronic up-regulation of MMP-13 expression in response to obesity-induced CLGI degrades the matrix of synovia, cartilage, and disc tissues in the joints of patients with OA, and causes fibrotic changes in liver tissues that drive cirrhosis and increases the risk of liver cancer. Now we can add to this growing body of research that chronic over-expression of MMP-8, stimulated by stress-induced CLGI, degrades the matrix of brain tissue in specific brain areas (especially the reward centers) causing depression-associated behaviors in animals.
This new research extends the body of evidence showing that CLGI, in part through its up-regulation of MMP, is a driver of many common psychiatric conditions, including depression, and identifies psycho-emotional stress as a second driver of CLGI. If this theory holds, then obesity and stress-induced CLGI may become the chief targets of lifestyle medicine, making mantra-based meditation like Transcendental Meditation (TM), which was recently shown to downregulate almost fifty different genes associated with inflammation, and the Modern Human Diet, which harnesses evolutionary biology to reduce visceral fat and lower inflammation, are among the most potent tools we have for preventing and treating many common chronic non-infectious diseases.